Medically reviewed by Misty Seidenburg
An elbow fracture is a break in the bone in the middle of the arm, near the elbow joint. It is a common injury, especially among children, women, and older adults. We use our arms for many simple and complex daily tasks, and an elbow fracture can make these movements difficult and painful.
Early physical therapy, occupational therapy, or hand therapy after a broken elbow is important. It not only helps speed healing and restore range of motion, but it also prevents stiffness and weakness, which can often develop if the arm is immobilized too long. By learning the signs of injury and the benefits of physical therapy, you can reduce pain and improve function, taking an active role in your recovery with elbow fracture treatment.
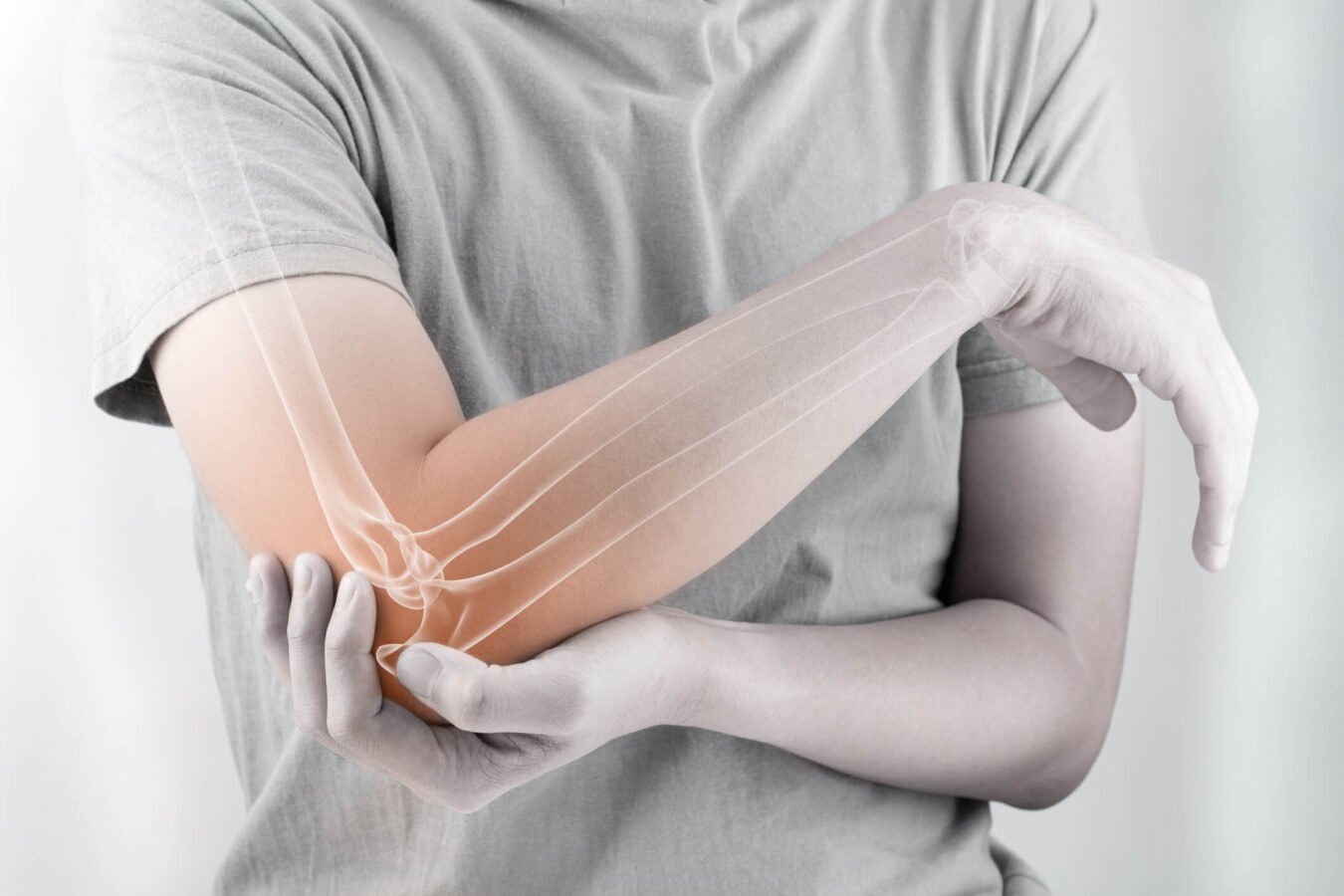
The elbow, a complex joint, is where the upper arm bone (humerus) meets the ulna and radius bones of the forearm. The ulna has a bony end called an olecranon, which cups the lower end of the humerus, creating a hinge for movement. The olecranon’s bony point, covered in a thin layer of tissue, is easily palpable. This joint’s intricate structure and function are crucial for our daily activities.
At the lower end of the humerus, the distal humerus forms a rod around which the forearm pivots as the arm bends and straightens. Muscles and ligaments support and connect these bones and nerves, crossing over the elbow to provide feeling and move muscles throughout the hands, arms, and shoulders.
A break in any elbow can cause considerable pain and impair mobility. Falls on the elbow or outstretched hands when the hands break the fall can cause a broken elbow. Car accidents, sports injuries, and other events that cause direct trauma to the arm near the elbow can also fracture these bones.
So, after an accident, how do you know there’s more to elbow pain than a minor bump or bruise? Common signs of a broken elbow include:
Do not ignore elbow pain after a fall. Proper treatment for elbow fractures is essential to prevent permanent complications and restore full function and mobility in the joint. If you suspect a fracture, see a healthcare provider to determine if you have one, the type of elbow fracture, and the proper course of treatment.
All elbow fractures are not alike. Treatment varies depending on the location and extent of damage. There are three main types of elbow fractures:
Fractures are considered displaced when bones are severely damaged and may have separated. In a non-displaced fracture, the bones remain in position. Providers physically examine the elbow and use advanced imaging tests, including X-rays, CT scans, and MRIs, to assess trauma and determine where and how severe the break is.
The first step in treating elbow fractures is to reduce the fracture or put the bones in the proper position to promote optimal healing and function. A closed reduction is performed without surgery. Treatment for non-displaced fractures may also include elevation, immobilization, and physical therapy.
Displaced elbow fractures may require surgery, called an open reduction, to realign the bones. Surgeons utilize screws, plates, and other surgical hardware to hold structures in place. In both cases, the patient may need a brace, sling, splint, or cast to stabilize the elbow as it heals.
Physical therapy is widely prescribed and recommended for elbow fractures that do not require surgery and as part of a post-operative rehabilitative protocol for patients post-surgery. It offers safe and therapeutic treatment to:
Elbow injury physical therapy protocols focus primarily on targeted exercises to build muscle strength and increase range of motion. Physical therapists combine exercise and stretching with massage and other safe and gentle hands-on therapies to reduce swelling and stiffness and promote tissue recovery.
Once patients are healed, physical therapists can shift to focus on fall prevention with balance and stability training, particularly for patients with higher fall risks, like older adults and those with mobility challenges.
Like fractured elbow symptoms, the recovery timeline for a broken elbow varies from patient to patient. Your physical therapist cannot determine the fractured elbow recovery time alone. They monitor your progress, and your healthcare provider follows up to assess your recovery and order imaging tests to determine if the break has fully healed.
After a broken elbow, your physical therapist is a vital member of your recovery team. They have the training and skills to facilitate your healing journey. Find a physical therapy clinic near you to schedule an evaluation for elbow pain today.
External Sources: